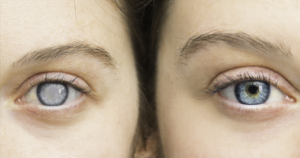
Glaucoma for most people isn’t noticed by a sudden flash of light or a painful warning sign that something is wrong. Instead, it is a slow, almost imperceptible narrowing of the world around the edges.
Understanding why this happens requires looking at the eye as a pressurised system. There is a clear fluid called ‘aqueous humour’ that constantly flows in and out of the front of the eye. When the drainage system gets backed up, much like a clogged sink, the pressure inside the eye begins to rise. This pressure eventually starts pushing against the optic nerve, which is the vital cable that carries visual information to the brain. Once those nerve fibers are damaged, they cannot be brought back, which is why early detection is the only real defense we have.
Spotting the Subtle Signs
The tricky thing about glaucoma is that the most common form, open-angle glaucoma, has virtually no early symptoms. You could have elevated eye pressure for years without feeling a thing. However, there is a less common type called acute angle-closure glaucoma that is much more aggressive.
This version can cause sudden blurry vision, severe eye pain, headaches, and even nausea or vomiting. Some people also report seeing rainbow-coloured halos around bright lights. If those symptoms ever appear out of nowhere, it is considered a medical emergency that requires immediate attention to save the eyesight. For everyone else, the symptoms are much quieter. It might start as a slight loss of side vision that you naturally compensate for by turning your head a bit more. This is why regular eye checkups are so critical, especially as we get older.
Why Does It Happen?
While high eye pressure is the primary driver, it is not the only factor. Some people have “normal-tension” glaucoma, where the optic nerve sustains damage even though the eye pressure is within the typical range. This suggests that some eyes are simply more sensitive or have poorer blood flow to the nerve.
There is also a strong genetic component to the condition. If a parent or sibling has been diagnosed, the risk for other family members increases significantly. Age is another factor, with the risk typically climbing after forty. Certain medical conditions like diabetes, high blood pressure, and even extreme nearsightedness can also play a role in how the drainage system of the eye functions over time.
Navigating Glaucoma Treatment Options
The goal of glaucoma treatment is to lower the eye pressure to a level where no further damage occurs. For most patients, the first line of defence is specialised eye drops. These work in one of two ways: they either help the fluid drain better or they tell the eye to produce less fluid in the first place. It sounds simple, but the effectiveness of these drops depends entirely on consistency. Missing doses can cause the pressure to spike, which puts the optic nerve back in the danger zone.
At specialised centres like Dr Agarwal’s Eye Hospital, the approach to clinical care is highly individualised. Surgeons look at the thickness of the cornea, the current state of the optic nerve, and the patient’s lifestyle before deciding which surgical or laser path is the safest bet.
The Role of Advanced Diagnostics
Tools like Optical Coherence Tomography (OCT) help doctors to spot the microscopic layers of the optic nerve. This allows them to track changes over time with incredible precision. If a nerve fiber layer is thinning by even a few microns, the technology catches it, allowing for a quick adjustment in the plan.
Living with the Diagnosis
Receiving a diagnosis of glaucoma can be unsettling, but with modern care, the vast majority of people maintain their vision for the rest of their lives. It requires a bit of a shift in mindset, viewing eye health as a long-term management project rather than a one-time fix. Consistently following your prescribed path ensures that the “silent thief” is kept at bay, preserving your sight for the years to come.